Before people ever get the chance to speak to you and get to know you, one of the very first things they will obviously notice about you is your face. Now everyone’s face is unique and special and should be properly cared for. The disease known as Shingles can affect the face and leave it looking scarred. Let’s take a look at how we can best avoid this from happening.

If you live to be 85 and above, then at some in your life you will probably have to face Shingles. Data reports estimate that one in every three people who live to that ripe old age, will have to face Herpes Zoster at some stage in their life. Most Shingles cases can be found in patients 50 years and older. So what exactly is this Shingles?
Shingles is a viral malady that is caused by the varicella zoster virus, the very same virus that causes chicken pox especially in young children [1]. And it can be a very painful disease too. Shingles can be also referred to as zoster. Painful blisters set on one half of the body typically identify this disease, with the rash appearing anywhere on the body, from the body torso right through to the face.
Transmission and Development of the Shingles Virus
Several things need to be noted about the transmission and developmental pattern of the Shingles Virus.
- The Shingles virus itself can be transmitted from someone suffering from the malady ONLY to an individual who has never had chicken pox before in their entire life.
- The virus is contracted through immediate contact with fluid that came from the Shingles blisters.
- The person who gets infected by the zoster virus will not develop Shingles immediately. Most likely they will develop chicken pox which clears off in about a month. But now that the person has the virus in their system, they could potentially develop Shingles, but much later on in life, perhaps decades later, or perhaps never.
- A person suffering from Shingles is only contagious when they are in the rash phase, after that or before the rash appears, they are not contagious.
- The zoster virus is never completely eliminated from the human body after someone has suffered from chicken pox. So if you suffered from chicken pox when you where a child, then the virus still resides in your body in a dormant form.
- The only reason the virus in your body doesn’t develop into Herpes Zoster is because of the strong immune system present which stops the virus from replicating out of control
- When the immune system becomes compromised however, the zoster virus takes full advantage and begins to multiply inside the body
- The virus lies dormant in the neural pathways of the body, so when it starts to multiply in the neural paths, this can cause disruption of the normal functioning of nerves and lead to some of the signs explained below.
How to Prevent Transmission to Others
There are simple steps that one can take out of courtesy to safeguard the health of others when one is suffering from the illness [2].
- Always keep the rash covered with a clean fresh bandage, and until it clears and avoid touching it as much.
- Desist from touching, scratching, patting the affected area.
- In the event that you have touched any affected areas, wash your hands, and in general it’s a good idea to wash your hands often.
- Avoid people who might have low immunities, this includes pregnant women, pre-term babies and people suffering from acquired immunodeficiency syndrome or people about to go for organ transplants.
General Signs and Symptoms of Shingles
It is important to understand that so long as the immune system remains strong, the sleeping virus in the nerves, for some people never gets active again but for some people, the virus is allowed to awaken from its dormant state because of a weak immune system. People prone to weak immunities include the elderly, injured persons and those on certain medication such as immune-suppressors. In the majority of cases, Shingles is a once a lifetime disease, although there are rare cases of some people who have recurring Shingles.
Herpes Zoster symptoms appear in a series of stages beginning with early stage and progressing all the way through to the full on Shingles illness.
- First phase involves mild headaches and sensitivity to bright lights. The headaches progress and in some people can become feverish in nature, and flu like symptoms are not uncommon.
- Then the itching and tingling sensations develop, and pain in several areas can be felt. The pain is as a result of the multiplied virus in the nerve endings.
- Feelings of dizziness and weakness can also accompany the pain.
- These early set symptoms can last anywhere from a day to three weeks before they progress into the infamous Shingles rash.
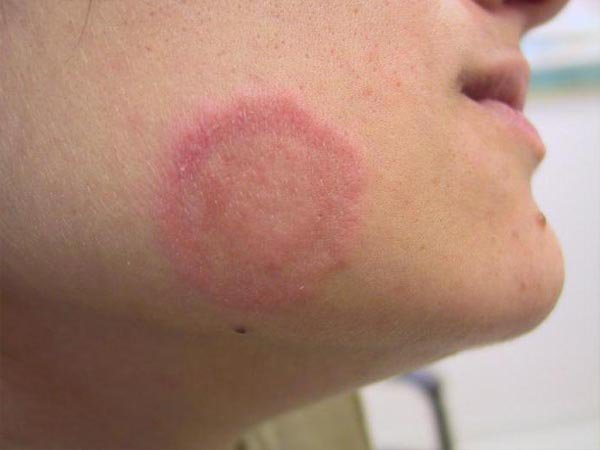
- The Shingles rash is a strip of rash. The rash consists of clusters of blisters that are fluid filled. As the days progress the blisters begin to crust or scab.
- Full healing from the blisters can take anywhere between two and four weeks. Scars may remain where the blisters used to be.
- Some individuals only develop a mild form of the rash , whilst some individuals do not even develop the rash, though they display all the other common Shingles characteristics.
It’s possible that you could also feel dizzy or weak. Or you could have long-term pain, rash on your face, changes in your vision, changes in how well you can think or a rash that spreads. If you have any of these problems from shingles, call your doctor right away.
How does Shingles infect face
Symptoms of Shingles on Face
Shingles in general can develop anywhere on the body. When it occurs on the face, it can prove to be problematic and it is important to handle it well to avoid leaving facial scarring.
The main facial areas affected are the eye area and mouth cavity [3]. When the Shingles affects the eye area, the virus can extend into the optic nerve and lead to serious cornea damage. When the virus enters the trigeminal nerve, this is the main nerve providing nutrients to the face area it can interact with and lead to the infection of the eye and mandibular nerve areas.
Like with the general symptoms, the symptoms affecting the face occur as a series of events:
- In the beginning the infection is identified by fever, pain in differing levels, tenderness and swelling of the nerves.
- Pain is commonly one sided and localised, meaning that it is either on one side of the face and not the other, leading many to feel a sense of imbalance.
- Painful blisters then begin to form along the length of the infected nerves, with the blisters in a delicate state and being able to break at any point causing deep cutting erosions in the dermis of the face. The damage done may be so severe that even after the herpes has cleared away some people are left to deal with facial paralysis, some even having to undergo speech therapy because of voice hoarseness, sores in the mouth amongst other unfortunate developments.
- Because it affects the nerves, and causes inflammation of the nerves, movement is extremely painful and tends to be of the excruciating kind. Post herpetic neuralgia may occur in some patients. Post herpetic neuralgia is the condition that may result because of nerve damage. It does heal but takes several months and some people even require years until they are able to fully function without the pain associated with this condition.
- The sensations often accompanying these inflammations include those of the tingling, prickling and itching type.
- If not properly attended to, the blisters can most certainly get infected by bacteria which would deter and slow down the healing process considerably. So it is important to keep the face area clean and clear of hair and makeup.
- In the mouth, herpes zoster will disrupt normal eating habits because if not properly taken care of, the nerves linking the mouth, the tongue, the pharynx and all the digestive and respiratory organs can be eroded and form lesions.
- When the nose develops a rash, then it is almost a pre-cursor to herpes zoster opthalmicus, herpes of the eyes.
- When Shingles reaches the eyes then it becomes worrying. Immediate attention must be considered because ocular shingles, affecting the eyelids and area surrounding the eye can lead to corneal damage, sensitivity to light and pain in the infected eye [4]. If not properly attended to, the blurring of the vision may occur and in extreme cases, blindness.
Diagnosis of Shingles on Face
In order to get a full and accurate diagnosis to be made by your physician, apart from the symptoms you exhibit, they must take samples of your tissue culture from the affected parts of your face and send them to the laboratories for further testing. Once the test results come back, then a full assessment can be done and the patient can start receiving treatment accordingly.
Treatment of Shingles on Face
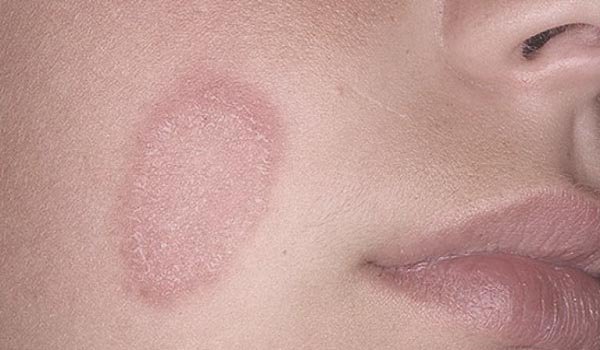
Shingles will naturally heal itself, but the physician may prescribe painkillers and/ antiviral medication to help ease the pain and soothe the affected areas. Treatment can last anywhere from several weeks to months depending upon the individual and the age of the individual. The elderly tend to take longer to heal.
The most common treatments include any combination of any of the following:
- For the unbearable pain; painkillers, whether prescribed or over the counter drugs, are your best source when seeking pain relief.
- Anti-viral medication is generally taken within the first 72 hours of the outbreak of a Shingles rash. People who have a tendency to have Shingles recur again tend to also take higher doses of antiviral drugs such as valacyclovir. The sooner this medication is started the better, because it will aid in the healing of the rash and the pain will equally be lessened.
- To completely shut off the pain in specific affected nerves, nerve blocks are used as anaesthetics, although their effect is short lived.
- Steroids as a rule of thumb are generally the last measure for Shingles. They do help in the reduction of inflammation and pain.
- The use of lotions such as calamine will help with soothing the affected face area. Oatmeal face masks and wet compresses can also work wonders to reduce the urge to scratch the blisters [5]. Keeping the face area clean is a top priority as you do not want the blisters to become infected by bacteria as well! The blisters may result in permanent scarring and patches in pigmentation so we want to make sure that we are doing the best we can to look after the face area.
- Finally, bed rest in the number one recommendation in order to heal faster. Eating well, resting and taking one’s treatment course as laid down by the physician is the fastest way to being whole and healthy again.
Shingles is a disease that will cure itself naturally, so it is important to remember that in the course of taking all the prescribed medications, you should rest adequately and help your body heal itself properly. It is important to take proper care of the area where Shingles has affected you. The face is a very sensitive area and so proper care should be taken in order to reduce the after effects of the disease. To avoid too much scarring, avoid scratching and picking at the scabs that form on your face. Avoid contact with your face, as your hands can carry bacteria, which if it gets into the lesions can cause yet another complication. Keep your face clean and covered with fresh bandages every day. Healing is just a matter of time, and does happen gradually. So you will simply need to be patient and not rush it.
Reference
[1] The New Journal of England: Use of an Inactivated Varicella Vaccine in Recipients of Hematopoietic-Cell Transplants, Hata, A., Asanuma, H., Rinki, M., Sharp, M., Wong, R. M., Blume, K., & Arvin, A. M.; N Engl J Med 2002; 347. Pp. 26-34 – July 2002 – DOI: 10.1056/NEJMoa013441 http://www.nejm.org/doi/full/10.1056/nejmoa013441
[2] Pediatrics: Varicella Prevention in the United States: A Review of Successes and Challenges, Marin, M., Meissner, H. C., & Seward, J. F. ; Volume 122 Issue 3. Pp. 744-751 – September 2008 – doi: 10.1542/peds.2008-0567 http://pediatrics.aappublications.org/content/122/3/e744.short
[3] A Journal of Neurology: The incidence and lifetime prevalence of neurological disorders in a prospective community-based study in the UK, MacDonald, B. K., Cockerell, O. C., Sander, J. W. A. S., & Shorvon, S. D. ; volume 123 Issue 4. Pp. 665- 676. – April 2000 – DOI: http://dx.doi.org/10.1093/brain/123.4.665 http://brain.oxfordjournals.org/content/123/4/665.short
[4] Aesthetic Surgery Journal: CO2 Laser Resurfacing: Recognizing and Minimizing Complications, Roberts, T. L., Lettieri, J. T., & Ellis, L. B. ; Volume 16 Issue 2. Pp. 142-148 – June 1996 – DOI: http://dx.doi.org/10.1016/S1090-820X(96)70038-9 http://asj.oxfordjournals.org/content/16/2/142.abstract
[5] Review of European Studies: Herpes Zoster: Description of the Associated Burden and Its Preventive Strategies, Lang, P. O. ; Volume 4 Issue 1. – 2012- DOI: 10.5539/res.v4n1p107 http://www.ccsenet.org/journal/index.php/res/article/view/15320
