Shingles is a painful infection which is caused by the virus known as Varicella zooster, the same virus which causes chickenpox [1]. Shingles is also called as Herpes Zoster in which the virus infects a nerve area and thus causes rash and pain along the area of skin supplied by the nerve which is affected. Shingles symptoms usually subside within 2 weeks to 6 weeks from the first appearance of symptoms. If the pain still persists after the rash disappears, then it can lead to painful complication which is hard to manage known as postherpetic neuralgia. Fortunately, this condition is quite rare and it occurs only in one out of five patients who suffer from Shingles.

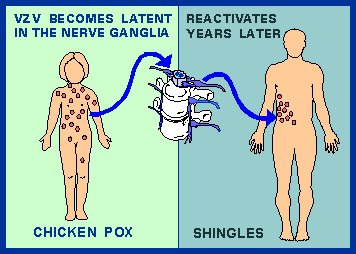
The Varicella Zoster virus remains dormant in every individual’s body who has suffered an episode of chickenpox in the past or those who have had the Varicella vaccine. While the dormant virus causes no harm to the body, in certain cases, the virus may be reactivated because of some external or internal stimulus. In such cases, the individual goes on to exhibit the signs and symptoms of the disease known as Shingles.
Shingles is a quite common infectious condition which is found to be more common in elderly people and more common in males. It is not a life threatening condition, but if the signs and symptoms of the disease are ignored and left without proper care, there is a high chance of complications occurring which can prove to be very serious.
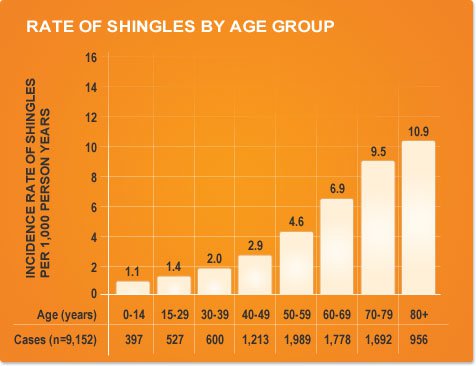
Shingles is also known to be associated to occur in individuals who have a weakened immune system and are exposed to the Varicella virus [2]. As such, individuals undergoing specific medical treatment, elderly people and other individuals who are suspected to have a weak immune system have higher chances of developing the condition.
Individuals typically only encounter a single episode of Shingles in their lives as the immune system of the body prevents any future onsets of the disease. However, in cases of individuals with a weakened immune system, Shingles may be experienced more than once in the lifetime. Even in such cases, it is quite rare for individuals to experience more than three episodes of Shingles in a lifetime.
It is important to seek medical recommendation at the earliest in case the signs and symptoms of Shingles are suspected in an individual. An early diagnosis of the infection may lead to a faster recovery and the chances of complications occurring are also averted. Shingles is also a highly contagious disease and as such, sufferers will need to take care so as to not infect other people around them.
Early signs of Shingles
If you have suffered from chickenpox in early life, then you might be aware of the typical signs of Shingles, which are more or less the same. The disease usually affects only a small area of the body on a single side of the torso. Some of the earliest signs and symptoms that accompany this disease are:
- Fever
- Headache
- Malaise
These early signs and symptoms are not adequate enough for the disease to be suspected. However, as with other viral infections, the symptoms keep manifesting themselves rapidly. The early symptoms are followed by the appearance of blisters on the surface of the skin. These blisters are often stretched out in a striped fashion on one side of the torso, or they may appear on one side of the face, one side of the neck, or they may affect the region surrounding one of the eyes. These blisters are really painful and also exhibit the following conditions as well
- Extreme sensation of itching
- A burning and painful sensation
- Hypersensitivity around the lesion area
- Numbness because of the pain and the rashes
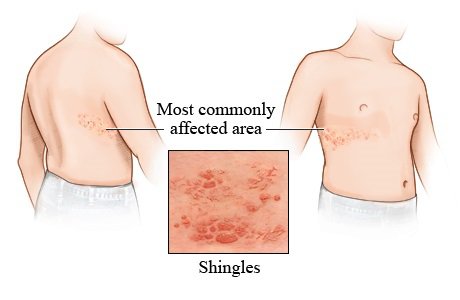
The most common site for the occurrence of pain and rash is either left or right side of torso. The rash forms a belt-like pattern, limited to only one side and not crossing the mid-line.
In some rarer cases of Shingles, there is no appearance of any blisters; however, the associated pain with the infection is present. In such cases, the pain is often misdiagnosed to have been caused by some other disease or underlying disorder.
Late symptoms of Shingles
Some of the later symptoms of Shingles which appear either after the onset of blisters and the earlier symptoms include the following:
- Formation of fluid-filled blisters over the rashes on the skin surface
- Darkening of painful vesicles
- Formation of and the falling off of crusts from around the skin lesions
If the early symptoms do not manifest and instead the later symptoms do, shingles may affect other areas of the body such as one side of neck or face or either of the eyes. In such cases, utmost care needs to be provided as these sensitive areas of the body are quite prone to suffer from complications. Complications may range from mild to severe and as such, must always be prevented.

Shingles may affect different individuals in different ways and the signs and symptoms may vary, as also the severity of the infection. However, typically, pain is almost always associated with Shingles. This pain is of a burning kind and is quite intense – so much so that many people even claim it to be one of the worst to be experienced in life.
Signs and Symptoms of Shingles in Children
In children, shingles is rare especially if they are less than 10 years of age. In case children are exposed to the Varicella Zoster, the chance of developing chickenpox rather than Shingles is much higher.
In young children, the symptoms of Shingle are much milder than those in adults [3]. While the symptoms typically manifest in themselves in the same way, the first burning sensation and rash are soon followed by formation of blisters. The only major difference in between the symptoms in adults and the symptoms in the case of children is that in the latter case, the symptoms are often painless. However, the formation of band on one affected area does occur.
Also, unlike in the case of adults, children rarely develop complications even if they encounter this disease.
Signs and Symptoms of Shingles in Pregnant Women
Shingles in pregnancy is quite rare, but there have been cases reported of pregnant women encountering the condition. The women who develop shingles in pregnancy have the same symptoms as those of adults but they face lesser chances of developing any complications.

However, pregnant women must always take care not to be infected with Shingles if possible. Not only will the condition be difficult to manage, but there may also be complications associated with the baby’s health in case Shingles is experienced during pregnancy.
Test and Diagnosis of Shingles
An early diagnosis of Shingles is required in order to both prevent complications as well as to enable a speedy healing and recovery time. While this may not always be possible, individuals who are suspected to be at risk or those who exhibit signs and symptoms of what is suspected to be Shingles should go for a diagnostic procedure.
The diagnosis of Shingles is typically done through an external examination as medical professionals are well-aware of what the symptoms of Shingles look like. However, it is always important to consider the medical history as also the family medical history, as well as to check for other underlying medical conditions before confirming the diagnosis of Shingles.
In some cases, a culture of the tissue are from around the blisters is examined in the laboratory to check for the presence of the Varicella Zoster virus. The tissue scrapings and fluid collected from blisters are sent to laboratory for diagnosis with the help of PCR. If the virus is found to be present, the blisters have been caused due to an infection of Shingles.
Additional testing of the culture is also carried out in order to determine if there are any chances of complications due to Shingles.
The diagnosis of Shingles is carried out by different types of medical professionals as per the different case of the condition [4]. The medical professionals could be any of the following:
- A general physician who is aware of what the symptoms of Shingles look like in case they manifest on an individual’s body
- A specialist consultant if an individual is already resorting to one for other medical conditions such as AIDS
- An eye specialist or ophthalmologist in case Shingles rashes and blisters affect the eye region
- A pediatrician in case the condition is developed by infants or babies
Complications of Shingles
Rare complications are seen in children and pregnant women affected with shingles. But in the case of older adults, if left untreated, the complications can become quite grave.
Perhaps, the most common complication associated with the disease is the development of post hepatic neuralgia, which is a painful condition involving several levels of the nervous system, thus becoming extremely difficult to manage. In such a case, the nerves of the individual are damaged due to the infection and they send out false signals of pain, as also exaggerated signals of pain. In such cases, even long after the symptoms of the disease subside, pain is felt by the individuals. The pain associated with postherpetic neuralgia can be described as exhibiting the following characteristics:
- A constant pain which is of the throbbing, aching and burning type
- Pain may be felt even by changes in temperature
- A hypersensitive condition to any type of pain
Postherpetic neuralgia can persist for quite some time in an individual. While typically the condition lasts for about three to six months, in some certain cases, it may last for many years and in others, it also proves to be permanent. This condition can be effectively managed with the help of painkillers, analgesics and other medications, but it is important to remember to seek proper medical consultation from a licensed professional before resorting to any medications.
Eye problems are also a common complication that is associated with the Shingles infection. In such cases, while the painful blisters may cause enough problems, other complications may arise if not managed properly. These complications include:
- Permanent scarring of the cornea and the appearance of sores along with ulceration
- Inflammation and damage being done to the optic nerve
- A buildup of pressure inside the eye leading to glaucoma
Complications associated with the eyes must be taken seriously or else they may worsen rapidly and may ultimately lead to a permanent loss in vision.
Another complication that is associated with Shingles is the case in which the nerves in the brain get infected. In such cases, individuals go on to develop the Ramsay Hunt Syndrome, a disease which is characterized by pain in the ears, dizziness, loss in hearing, episodes of vertigo, appearance of rashes around the ears, a loss in the taste palette, weakening of the face muscles and also a feeling of tinnitus. Fortunately, this disease can be treated with the help of corticosteroid drugs or antiviral medication. In case the condition is not attended to, the patients may suffer from permanent hearing loss or permanent facial paralysis.
Some of the other complications that are associated with the Shingles infection include [5]:
- Scarring around the area of the rash and the blisters, often accompanied with a loss of pigmentation and whitening of the skin
- Rashes and skin lesions are quite prone to being infected by bacteria
- Inflammation of other organs of the body such as the lungs, the liver, the brain, the spinal cord and also the membranes protecting the spinal cord and the brain may occur
Complications associated with Shingles are much more common in cases in which the sufferer has had blisters over the neck, face or around the eyes. While these blisters prove to be not only difficult to manage, extreme care must be taken in order to prevent any chance of complications. As such, if these typical symptoms of Shingles manifest themselves, proper medical attention must be provided at the earliest.
While Shingles by itself is not considered to be a life threatening condition, the complications can prove to be quite severe.
References
[1] The FACEB Journal: Infection by human varicella-zoster virus confers norepinephrine sensitivity to sensory neurons from rat dorsal root ganglia, Kress, M., & Fickenscher, H. ; Volume 15 number 6. Page 1037-1043 – April 2001 – DOI :10.1096/fj.00-0440com http://www.fasebj.org/content/15/6/1037.short
[2] Annual Reviews of Virology: Live Attenuated Varicella Vaccine, Arvin, A. M., & Gershon, A. A.; Volume 50. Pp. 59-100 – October 1996 – DOI: 10.1146/annurev.micro.50.1.59 http://www.annualreviews.org/doi/abs/10.1146/annurev.micro.50.1.59
[3] Family Practice: Herpes zoster and postherpetic neuralgia: incidence and risk indicators using a general practice research database, Opstelten, W., Mauritz, J. W., de Wit, N. J., van Wijck, A. J., Stalman, W. A., & van Essen, G. A. : Volume 19 Issue 5. Pp. 471-475 – May 2002 – doi: 10.1093/fampra/19.5.471 http://fampra.oxfordjournals.org/content/19/5/471.short
[4] A Journal of Neurology: The incidence and lifetime prevalence of neurological disorders in a prospective community-based study in the UK, MacDonald, B. K., Cockerell, O. C., Sander, J. W. A. S., & Shorvon, S. D.: Volume 123 Issue 4. Pp. 665-676 – April 2000 – DOI: http://dx.doi.org/10.1093/brain/123.4.665, http://brain.oxfordjournals.org/content/123/4/665.short
[5] America Journal of Epidemiology: Comparing Shingles Incidence and Complication Rates From Medical Record Review and Administrative Database Estimates: How Close Are They?, Yawn, B. P., Wollan, P., & Sauver, J. S. ; Volume 174 Issue 9. Pp. 1054-1061 – September 2011 – doi: 10.1093/aje/kwr206 http://aje.oxfordjournals.org/content/174/9/1054.short
